
Diet and Cancer: What Have We Learned?
by Laurence Kolonel, M.D., Ph.D., Deputy Director, Cancer Research Center of Hawaii, Honolulu
In the mid-1970s, the U.S. National Cancer Institute initiated a Diet and Cancer Program to support investigations in this largely unexplored area. Over the last 25 years, scientific reports on nutrition and cancer relationships have appeared with increasing frequency. What has this body of research revealed?
An Historical Perspective
Many of the earliest studies in the field of diet and cancer were ecologic, examining correlations between cancer rates and cross-sectional dietary exposures, generally based on dietary surveys or national food consumption data and corresponding incidence or mortality rates. Among the earliest was a study by Armstrong and Doll in 1975, which suggested that higher consumption of meat might predispose to colon cancer and that higher intake of dietary fat might predispose to breast cancer.
Subsequent studies emphasized the case-control approach, in which patients with particular types of cancer and suitably matched controls were interviewed about their diets prior to the onset of the disease. Because dietary recall can be biased (inadvertent overestimation or underestimation by cases relative to controls), many investigators initiated large prospective cohorts, such as the renowned Nurses Health Study at Harvard University and the Cancer Prevention Study of the American Cancer Society, as well as the more recent Multiethnic Cohort Study of Diet and Cancer, and the European Prospective Investigation into Cancer and Nutrition (EPIC). While much more costly, these studies obtain dietary information from subjects prior to the onset of illness, thereby obviating the potential recall bias of case-control studies.
Increasingly frequent reports from cohort studies since the 1990s have been crucial to establishing most of the diet-cancer relationships noted below. Although intervention studies (randomized control trials) are considered the ultimate means to explore the relationship of an exposure like diet to cancer, such investigations also have limitations and are rare, due to their enormous cost, difficulty to implement, and the impracticality of testing more than a single exposure level in one study.
Can Diet Increase Cancer Risk?
Many early case-control studies suggested a role of dietary fat, especially saturated fat, in the etiology of cancers at several sites, especially the breast, prostate and colorectum (large bowel). Because the major sources of saturated fat in most Western diets are meat (notably red meat) and whole dairy products, these food groups in particular were implicated. However, subsequent cohort studies have been less supportive of this association. Furthermore, a 2006 report from an intervention trial, the Women’s Health Initiative, failed to show a reduced risk of breast or colorectal cancer in women who followed a low-fat diet (though the women only maintained an average fat intake of 29 percent of calories, which is not particularly low). Thus, the role of dietary fat per se in these cancers remains unclear. Nevertheless, there is a strong biologic rationale for such an effect, and supportive data from animal studies, so the hypothesis remains viable.
Other dietary constituents that may increase the risk of cancer include the heterocyclic amines and polycyclic hydrocarbons formed in meats cooked at high temperature or charcoal-broiled, and nitrosamines that can be formed from foods preserved with nitrates or nitrites (such as processed meats). An established carcinogen for humans is aflatoxin, a substance produced by molds that can contaminate improperly stored ground nuts, legumes and grains.
Obesity, which reflects an energy imbalance in the body, is clearly associated with several cancers, including those of the colon, endometrium, breast (in postmenopausal women), lower esophagus, kidney and gallbladder. And obesity is a growing global problem. Today, in the United States alone, more than 60 percent of adults are estimated to be overweight, with half of them classified as obese. And the developing world has not been spared: Obesity rates in India are now estimated at 15 percent.
Can Diet Lower Cancer Risk?
Vegetables, especially raw or minimally cooked, and to a lesser extent fruits, have been consistently associated with lower risks of many cancers, including those of the lung, esophagus, stomach and colorectum. Vegetables and fruits contain fiber, vitamins, minerals and a variety of non-nutritive constituents, such as carotenoids, flavonoids, indoles and sterols, all of which could account for this protective effect.
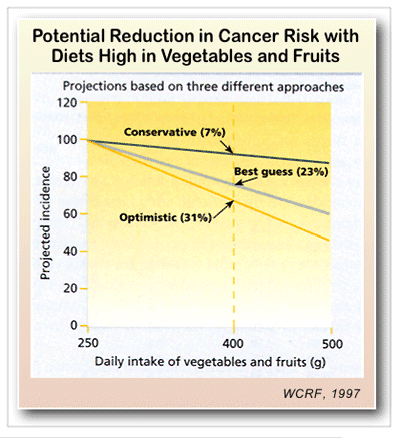
The reduced risks associated with vegetable and fruit consumption have been consistent in case-control and cohort studies, although the few intervention studies reported to date have yielded somewhat mixed findings. An expert panel of the World Cancer Research Fund (WCRF) reviewed the evidence on diet and cancer in 1997 and estimated the potential reduction in cancer risk achievable by increasing the consumption of vegetables and fruits (see figure). The figure shows three sets of projections – optimistic (maximal), middle-ground (average) and conservative (minimal) – of the effects of increased daily intakes of vegetables and fruits on overall cancer risk. Using the middle-ground projections, the incidence of cancer could be reduced by more than 20 percent with an average vegetable/fruit intake level of 400 grams/day (as recommended by WHO/FAO). If the average intake were increased to 500 grams/day, the incidence of cancer could be reduced by an estimated 40 percent.
Consumption of whole grains has also been related to lower cancer risk, perhaps because these foods too contribute fiber and other micronutrients to the diet and are relatively low in caloric density. Although dairy foods can add fat to the diet, as noted above, they are also an important source of calcium, which has been identified as a protective factor for colorectal cancer in many studies. Low-fat and skim dairy products provide calcium without increasing saturated fat intake.
Another important protective factor indirectly related to diet through its effect on energy balance is physical activity. Even in moderate amounts, physical activity has consistently shown a benefit in reducing the risk of colorectal and post-menopausal breast cancers, with more limited evidence for some other sites.
The Jury is Still Out
Among the many reasons for the lack of clear and consistent associations between diet and cancer are the difficulties in valid assessments of dietary intake in free-living populations with access to an enormous variety of foods, the changing patterns of eating over time, and the complexity of the exposure (thousands of different constituents in foods, different methods of cooking and storing foods, etc.).
A more recently recognized complexity is variation in susceptibility among individuals and groups. Currently, research is underway to identify such inherited susceptibility factors and to study diet-gene interactions that may help to clarify associations between food intake and cancer. In 1997, for example, Le Marchand and colleagues in Hawaii showed that Japanese-Americans who consume their meats well-done are more susceptible to colorectal cancer than Caucasians, because they are more likely to carry a variant form of the gene that metabolizes the heterocyclic amines that form in foods cooked at high temperatures.
Whereas the effects of individual dietary components on cancer risk are relatively small (i.e., individuals with high exposures may have twice (or half) the risk of those with low exposure), food is a universal exposure, and the number of persons whose cancers can be attributed to adverse dietary exposures is enormous. Indeed, diet has been variously estimated to account for some 30 percent of the cancer burden in most populations. Nutrition is essential to life, however, so blanket elimination of the exposure as a cancer control measure is not an option.
Paradoxically, at a time when sedentary behavior has dramatically increased in most societies, food portions, both within and outside the home, have expanded. Reducing portion sizes and appropriately adjusting the ratio of meat to vegetables and grains on a typical plate can have an enormous impact on intake.
Modest Dietary Changes Could Reduce Risk
Cancer is a major public health burden in both the developed and developing world. In 2002, the estimated number of incident cancer cases globally was nearly 11 million, with about 40 percent of these in developing regions of the world. Many organizations, such as the WCRF, the World Health Organization (WHO) and the U.S. Department of Health and Human Services, have produced dietary guidelines to lower the risk for cancer (and other chronic diseases). All essentially reach the same conclusions, as summarized in the following table:
Comparison of Dietary Recommendations for Cancer Prevention with Those for
Chronic Disease Prevention & Health Promotion
Food Groups or Nutrients |
Diet and Cancer Prevention WCRF, 19971 |
Diet & Chronic Disease Prevention WHO/FAO, 20032 |
Dietary Guidelines for Americans USDA/DHHS, 20053 |
| Fruits and vegetables | Select mostly plant-based diet. = 5 servings fruits & vegetables | At least 400g | Sufficient fiber-rich fruits & vegetables from all 5 groups |
| Meat, Poultry & Fish | Limit red meat to <3oz./d & <10% energy. Choose fish & lean poultry | No specific recommendation | Select lean meat, poultry, fish |
| Milk & Milk Products | No specific recommendation | No specific recommendation | = 3 cups fat-free or low-fat milk or milk products |
| Fats, Oils & Fatty Foods | 15-30% a .Limit fatty foods & oils, especially of animal origin | 15-30%; < 10% SFA 6-10%PUFAb; < 1% Trans fats; <300 mg cholesterol/d | Limit fats & oils to 25-30% ; < 10% SFA <300 mg cholesterol. Trans fats as low as possible |
| Carbohydrates (% total energy minus protein and fat) | 45-65% energy = 7 servings minimally processed grains, legumes | 55-75% energy especially from whole grains (remaining 10-15% from protein) | = 3 whole grain servings; also consume dry beans |
| Total dietary fiber | 38g and 25g for men and women = 50 years | > 25g preferably from whole grain foods | Choose fiber-rich foods |
| Free sugars | Limit consumption | < 10%c | Limit added sugar & caloric sweeteners |
| Alcoholic Beverages –if consumed | Not recommended. Limit to 1 drink for women & 2 for men | No specific recommendation | Limit to 1 drink for women; 2 for men. Avoid during pregnancy & lactation |
| Sodium chloride | <6 g. Limit salted foods | 5 to 6 g (iodized) | < 2300 mg sodium (~1 tsp) |
| Dietary Supplements | Probably unnecessary, possibly unhelpful for reducing cancer risk | No specific recommendation | No specific recommendation |
| Food Hygiene, Cooking & Storage | Refrigerate perishable food; avoid eating contaminated food; Avoid charring foods | No specific recommendation | Practice good food hygiene. Avoid consuming raw or undercooked meat, poultry, eggs & dairy foods. |
| Body Weight | BMI 18.5-25. Limit weight gain in adulthood to 11 lbs. | Avoid obesity. BMI 18.5-24.9. Limit lifetime weight gain to 11 lbs. | Balance caloric intake and expenditure; prevent weight gain through exercise |
| Physical activity of moderate intensity d | 60 min. brisk walk daily; =60 minutes vigorous activity/week | At least 30, pref. 60, minutes daily | 30-90 minutes moderate-vigorous activity several times/week |
1. World Cancer Research Fund/American Institute for Cancer Research: Food, Nutrition and the Prevention of Cancer, Washington, DC 1997; 2. World Health Organization: Diet, Nutrition And The Prevention Of Chronic Diseases. Report of a Joint FAO/WHO Expert Consultation. WHO Technical report Series 916. WHO, Geneva, 2003; 3. USDA/DHHS: Dietary Guidelines for Americans 2005. Government Printing Office, Washington, DC, 2005.
a Percentages refer to proportion of total daily energy consumed.; SFA=saturated fats. b 1-2% of the PUFAs as n-3 PUFA.; c All added monosaccharides and disaccharides, plus sugars naturally present in honey, syrups and fruit juices d Recommended duration varies with focus: cardiovascular risk reduction or weight reduction.
Although present evidence to support these recommendations is not definitive, the guidelines are prudent, almost certainly will do no harm, and are unlikely to change substantially as knowledge in this area grows. Furthermore, the relationship between diet and cancer is totally consistent with that for other chronic diseases, such as coronary heart disease, stroke, diabetes and hypertension.